One afternoon, during my intermediate student life at MC College hostel, I was studying for class. Suddenly I started feeling down, without any reason. Nothing bad had happened, but something didn’t feel right. Then I remembered, I’d also been having digestive issues for a few days.
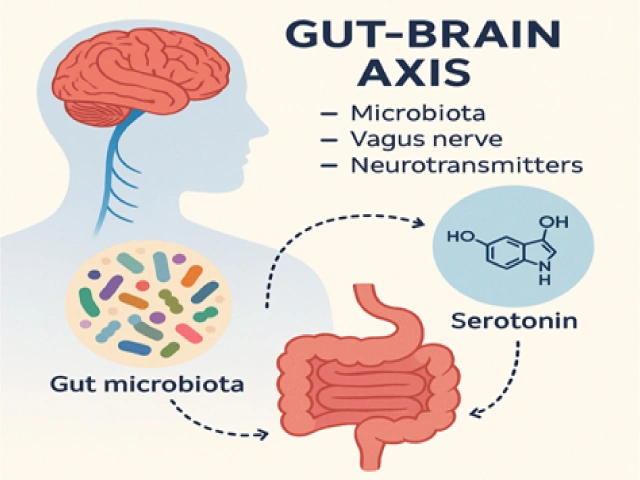
This small incident introduced me to a fascinating concept—the Gut-Brain Axis, the deep neurobiological connection between the gut and the brain. Modern research suggests that the trillions of bacteria living in the human gut influence not just digestion, but also our emotions, decisions, and even mental states such as depression!
Research Paper Review: “The Psychobiotic Revolution” and Cryan’s Work
In 2011, renowned researcher John F. Cryan and his team showed in the article “The Psychobiotic Revolution” that gut bacteria—especially ‘Lactobacillus’ and ‘Bifidobacterium’—play a vital role in mood regulation, stress response, and memory formation. They noted that neurotransmitters produced by gut bacteria, such as serotonin, GABA, and dopamine, send signals directly to the brain.
One significant point: 90% of the serotonin produced in our body is made in the gut. Cryan says, “The gut talks to the brain more than the brain talks to the gut.” These signals reach the brain via the vagus nerve, which works like a kind of neuronal highway.
Research shows that people suffering long-term from irritable bowel syndrome (IBS) or gastrointestinal issues tend to have a significantly higher tendency towards anxiety and depression. This proves that not just our mental states, but decision-making, risk-taking behavior, and even social interactions can depend on the gut.
Diving Deeper: The Role of Inflammation and Immune Response
The gut-brain axis is not limited to just nerve signals; the immune system and inflammation also play major roles here. Research shows that when intestinal permeability increases (known as “leaky gut”), certain toxic molecules can traverse into the bloodstream abnormally.
These molecules reach the brain and trigger neuroinflammation, which can heighten the risk of depression, autism, and even Alzheimer’s disease. For example, a 2020 study published in Nature Neuroscience found that molecules called lipopolysaccharides (LPS), which are produced by some harmful bacteria, can enter the brain and activate microglial cells. This then starts a process of long-term inflammation in the brain, impacting mood, cognition, and behavior.
Hormones and the Gut: Further Amazement
Gut bacteria influence not only neurotransmitters, but also the secretion of various hormones. Research shows that the gut microbiome can affect cortisol (the stress hormone), ghrelin (the hunger regulator), and even oxytocin (the hormone involved in building social bonds). So, digestive imbalance affects not only our mood, but also our habits, appetite, and even feelings of love and affection.
What Can We Infer?
The gut microbiome, known as the body’s “second brain,” is more than just a digestive factory. It is a key orchestrator of our feelings and behaviors. In the future, treating depression or mental disorders might not just rely on medication, but may see probiotic-based therapy as a revolutionary solution.
Researchers are even working on a new class of probiotics called psychobiotics, designed to target specific psychological symptoms. A 2022 study in Cell Reports stated that some bacteria produce odorants that can directly stimulate the limbic system—the brain area governing emotions.
New Discussion Angle: Personalized Microbiome Therapy
New research states that every person’s gut microbiome is unique. So, future treatment might be based on personalized microbiome analysis and corresponding probiotic or prebiotic therapy. For example, a 2023 Harvard Medical School study found that certain deficiencies in gut bacteria prevent antidepressants from working. That study recommends that gut analysis could be a crucial step before treating depression.
Mental Clarity or ‘Brain Fog’— The Gut’s Deeper Shadow
Have you ever experienced this—you’re in class, eyes open, the teacher is teaching, but your mind feels somewhere else? You’re not tired, nor sleepy. Yet it’s like there’s a mental mist clouding over you. This mysterious sensation is called “Brain Fog”—a kind of mental haziness that slows down decision making, focus, and memory power.
Now the question is, is this merely a brain disorder? The answer: no. Modern neuro-gastroenterology suggests the root often hides deep in our gut, especially in imbalances of the gut microbiome.
Unhealthy Diet and Microbiome Destruction
Nowadays, students and working people’s diets are full of processed foods, trans fats, high sugar, and artificial preservatives. These destroy the beneficial bacteria in the gut and support the growth of harmful bacteria.
Research (Frontiers in Neuroscience, 2017) shows that regular eating of processed food reduces the levels of ‘Firmicutes’ bacteria in the gut—a group that primarily helps prevent inflammation in the body and contributes to serotonin production in the brain. This dysbiosis—or abnormal bacterial balance—results in mental haziness.
‘Leaky Gut’ and Neuroinflammation: Across a Thin Bridge to Depression
When gut bacteria lose balance, intestinal permeability increases. This state is called “Leaky Gut,” through which food or bacterial toxins can enter the bloodstream.
When these toxins (especially lipopolysaccharides or LPS) reach the brain, microglial cells (the brain’s immune cells) get activated, initiating neuroinflammation. That’s when symptoms such as “brain fog,” poor attention, and trouble with decision making appear.
A famous study (Harvard Medical School, 2020) reports that people with IBS or GI issues have comparatively lower cognitive performance, one major reason being this chronic low-grade inflammation.
The Haze on Memory: The Gut’s Invitation
Gut bacteria help produce a neurotrophin hormone called BDNF (Brain-Derived Neurotrophic Factor). This hormone is vital for generating neurons in the brain and preserving memory.
But when the gut flora is weak, BDNF levels drop. This raises the risk of memory loss, difficulty recalling words, or suddenly forgetting simple things. These symptoms are part of the so-called “brain fog.”
How can you recognize these symptoms?
1. Suddenly unable to concentrate in class, easily distracted
2. Unable to read continuously, needing to reread repeatedly
3. Delay in recalling something
4. Getting stuck on words while speaking
5. Head feels heavy, vision seems clouded like mist
How to Control This ‘Brain Fog’?
1. Plant-based diet: Lots of fiber and probiotic-rich foods like yogurt and fermented foods increase beneficial gut bacteria.
2. Anti-inflammatory foods: turmeric, ginger, green tea, etc., reduce inflammation in both gut and brain.
Mindfulness and meditation: These enhance vagus nerve activity on the gut-brain axis, increasing focus.
Avoiding unnecessary antibiotics: This prevents destruction of helpful gut flora.
Some Messages: Find Light Within to Dispel the Fog
‘Brain Fog’ is not an imaginary mental issue, but rather a biological chemical signal rising from our gut. The brain and gut are like a two-headed creature, where even the smallest change echoes at the other end. To improve future learning or professional productivity, caring for gut microbiome will be the wisest decision.
What do your thoughts say?
Md. Iftekhar Hossain
Medical student, Cox’s Bazar Medical College | Interested in neuroscience, habit formation, and behavioral change in the human brain.










Leave a comment