Zainul Abedin Sagar
MBBS (Final Year),
Mymensingh Medical College
An Ordinary Story, an Overwhelming Crisis
It was last winter. I went home to Gurudaspur in Natore during the holidays. One evening, Uncle Hasan from the next house (name changed) called me over. His son had been suffering from a fever for several days. He had been giving him ‘Ciprofloxacin’ from the local pharmacy. The fever didn’t go away; instead, his son now also had bloating and increased weakness.
I asked, “Have you gone to see a doctor?”
He replied, “What’s the point? Last time this antibiotic worked just fine.”
This is a very common scenario. But it’s terrifying. Because like this boy, thousands of children, elderly, and young adults are being infected every day by bacteria that have become used to these medicines—bacteria that no longer respond to any available drugs.
Antibiotic Resistance—In Simple Terms
Antibiotic Resistance (AR) means antibiotics no longer cure infections the way they used to. That’s because bacteria have adapted themselves so well that these drugs can’t kill them anymore.
Every time we take antibiotics unnecessarily or give them to others, we are teaching those bacteria “how to survive.” And that’s how superbugs are born. (Superbugs are germs—like bacteria & fungi—that cause hard-to-treat infections.)
Numbers That Frighten Us
- Deaths worldwide due to antibiotic resistance in 2019: 1,270,000. (The Lancet)
- Projection: By 2050, more than 10 million people will die each year.
- In Bangladesh, 70% of antibiotics are used without a prescription.
- One study found that in clinics outside Dhaka, 90% of patients with fever were given antibiotics—even though most cases were viral fevers.
The Reality of Rural Healthcare
I’ve seen firsthand that in our village, every pharmacy owner seems to act like a doctor. Some haven’t even finished school, yet they diagnose patients and say, “Just take this and you’ll be fine.”
When a laborer gets sick, their first stop is the pharmacy—because it’s cheaper, and there’s no doctor’s fee. The shopkeeper says, “Take Ixin (Cefixime); you’ll be fine in two days.”
But what really happens is that only half the bacteria are killed. The rest make themselves at home in the body, learn to recognize the medicine, and next time that drug doesn’t work at all.
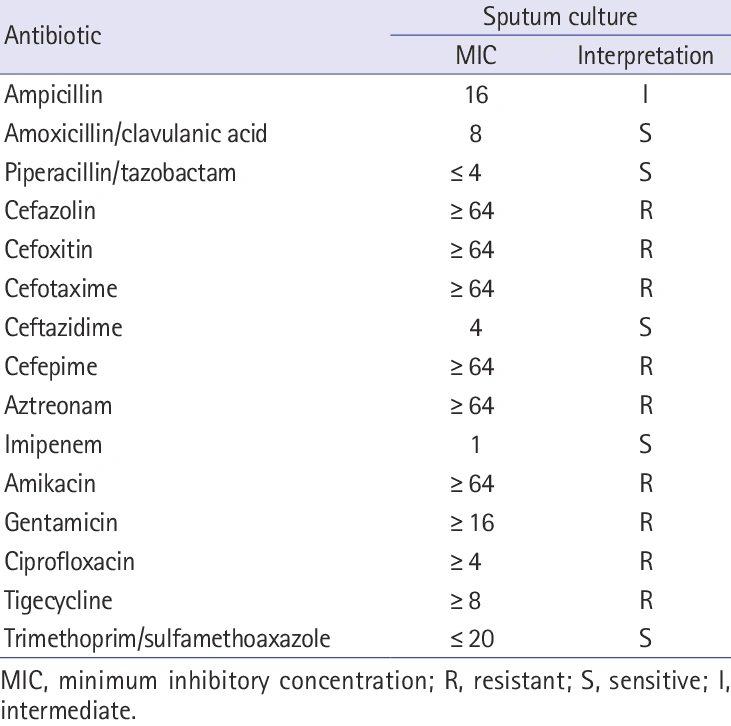
Superbugs—Monsters of Our Own Making
Once during a clinical class in the ward at Mymensingh Medical College Hospital, I saw a case—a 25-year-old woman admitted with a urinary tract infection (UTI). Our professor prescribed one antibiotic after another, but nothing worked. Lab reports revealed the bacteria was ESBL positive, a type that doesn’t respond even to regular antibiotic injections, let alone oral medicines.
A Mother’s Tears
My roommate’s uncle works at ICDDR,B Hospital. One day, he shared, “A mother spent 7 days wandering from one hospital to another with her sick child. Each place said it was an infection, but no medicine worked. Finally, when the child was admitted to the ICU, a blood culture revealed: Carbapenem-Resistant Enterobacteriaceae (CRE)—for which no hospital in the country has any effective drug.”
He said he still can’t forget that mother’s tears.
Where Are We Going Wrong?
- Taking antibiotics for viral fevers.
- Stopping antibiotics after three days just because we “feel better.”
- Mixing excessive antibiotics in poultry and cattle feed.
- Giving ‘Ciprofloxacin’ injections to children for a simple fever.
- Not using gloves or hand sanitizers in hospitals.
What Is the World Doing? What Are We Doing?
World:
- WHO launched the ‘Global Action Plan on ARM’.
- In England and Sweden, antibiotic use has dropped by more than 30%.
- MIT and DeepMind are using AI to discover new antibiotics.
Bangladesh:
- ICDDR,B and BMRC are conducting research on antibiotics.
- Some medical colleges have launched ‘Antibiotic Stewardship Programs’.
- DGDA has started work on regulated antibiotic sales laws.
But the reality?
In rural areas, still no one knows what ‘Antibiotic Resistance’ is…!
What Should We Do?
- Don’t take antibiotics without the advice of a registered doctor.
- Don’t leave your antibiotic course incomplete.
- Don’t give your medicines to others.
- Stop the overuse of antibiotics in animal feed.
- Raise awareness within your family and community.
A Final Word for You…
When humans discovered antibiotics, it was a triumph for life.
Now we are destroying that life-saving weapon ourselves simply due to uncontrolled use.
Soon, even common colds and fevers may become deadly.
Our children might one day wonder—“Was there really a time when people didn’t die from infections…?”
Are we heading towards that uncertain future???
References
- The Lancet (2022): Global Burden of Bacterial AMR
- WHO Fact Sheet on Antimicrobial Resistance
- ICDDR,B Bangladesh AMR Data
- CDC – Antibiotic Use in South Asia
- BMRC Report on Drug Misuse, 2023
- UNICEF: Rural Drug Practice in Bangladesh
- Review on Antimicrobial Resistance (UK, 2016)











Leave a comment